
Key findings
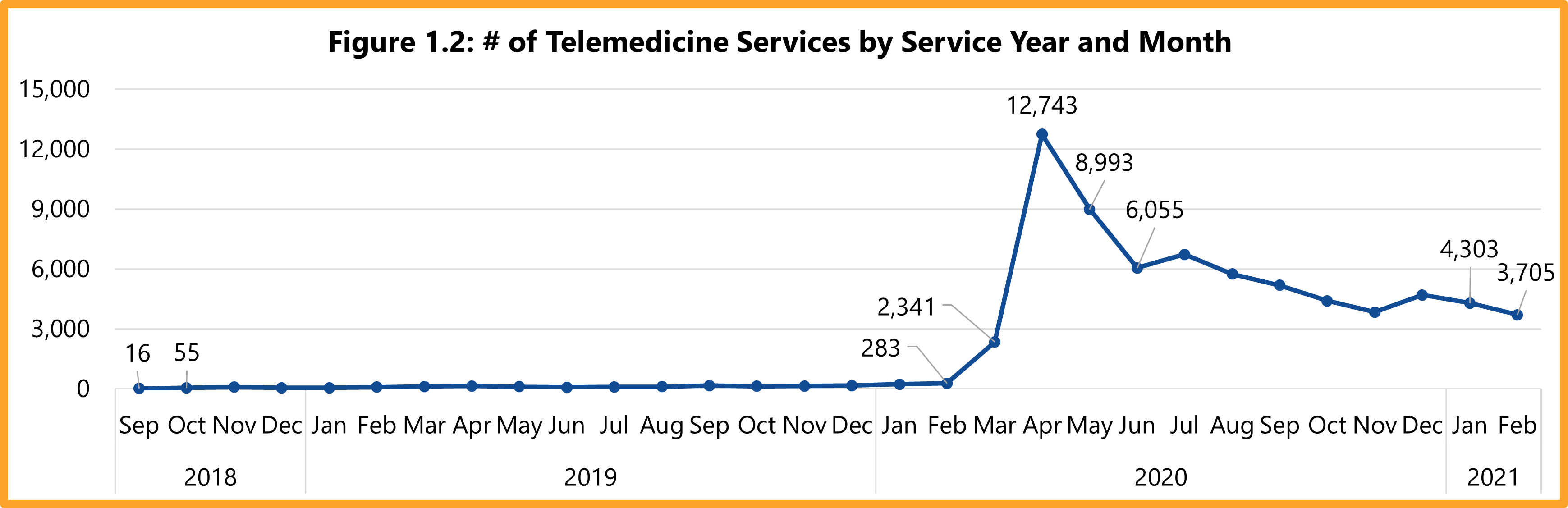
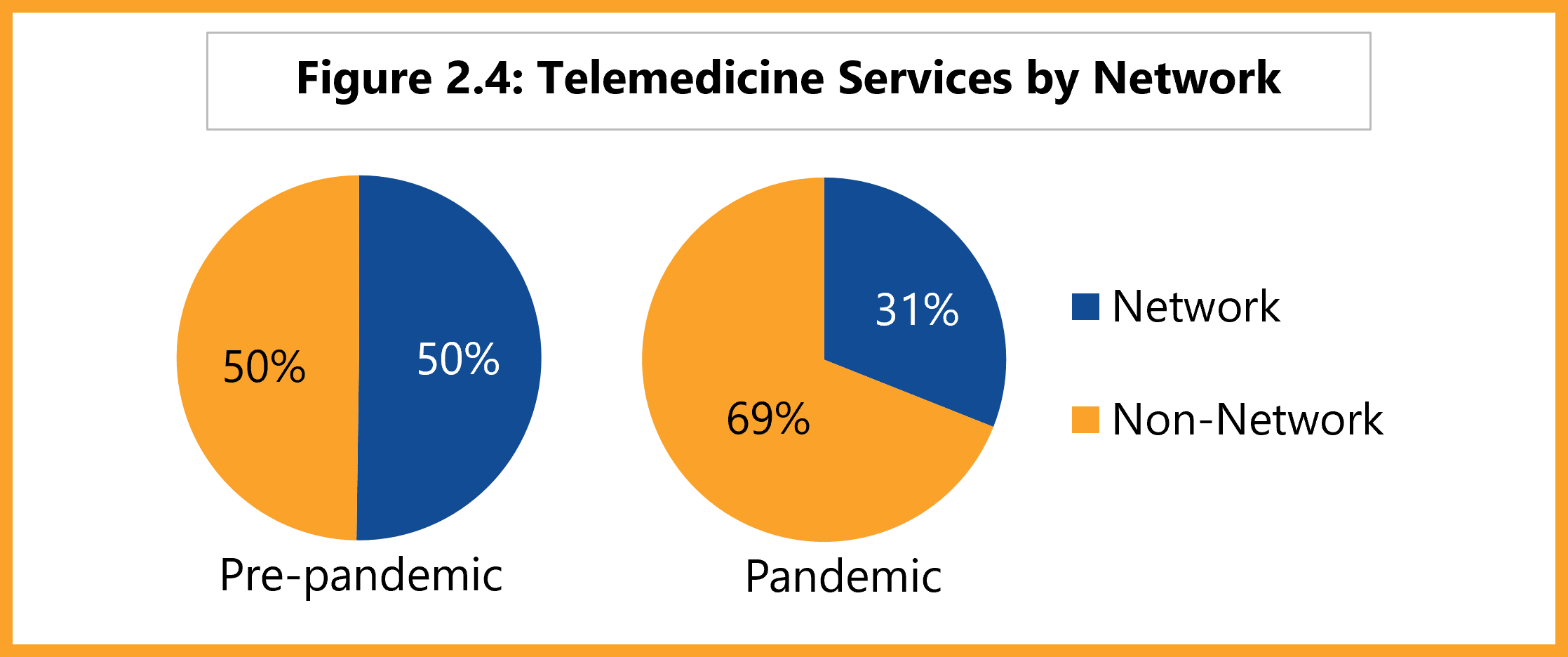
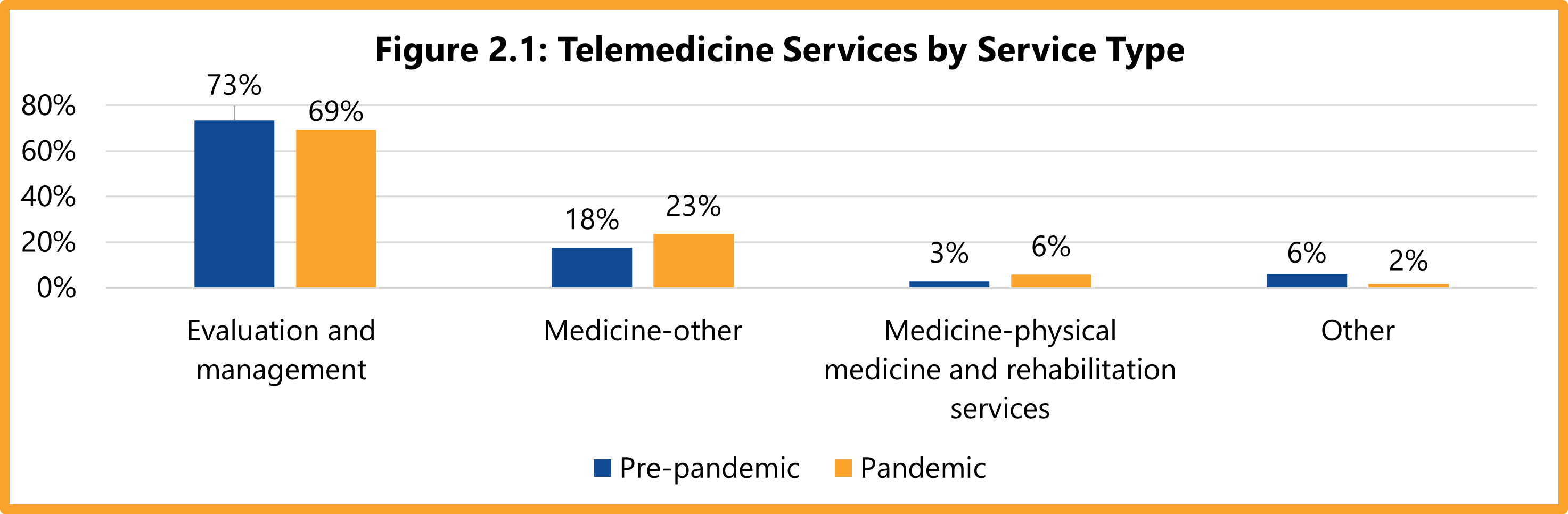
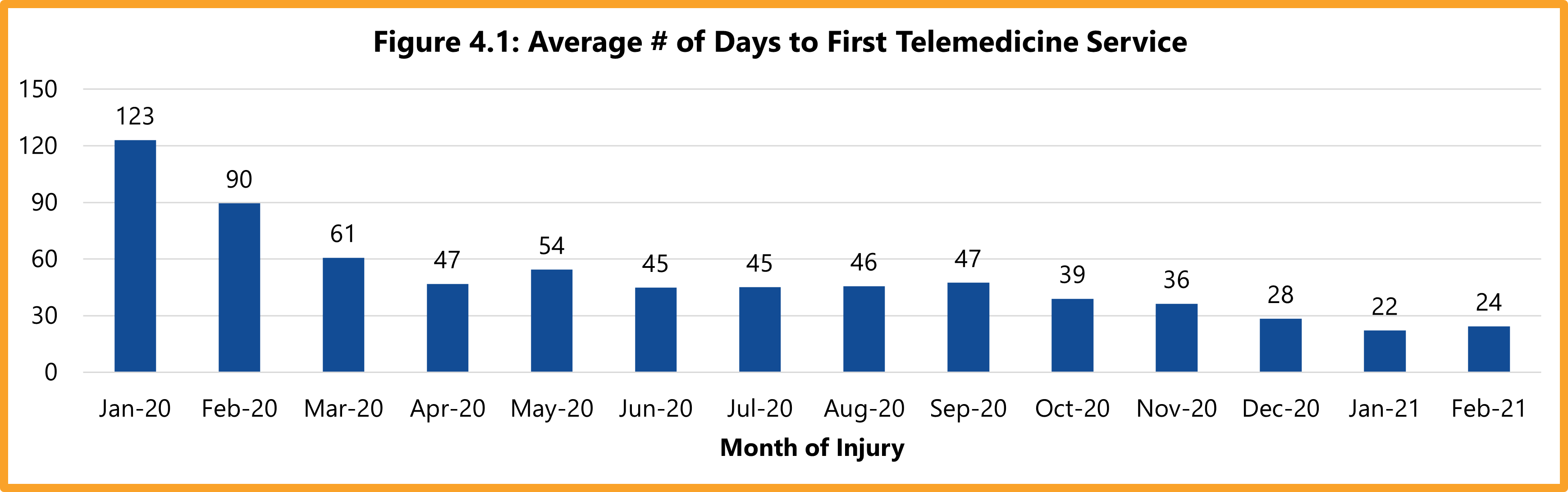

DWC adopted 28 Texas Administrative Code §133.30 on September 1, 2018, in an effort to expand injured employees’ access to telemedicine services. This report examines trends in telemedicine services in the Texas workers’ compensation system since 2018. Specifically, this report compares the use and cost of these services before and during the COVID-19 pandemic. The report also compares telemedicine use for network and non-network claims. Findings from this report provide a baseline to track future changes in the utilization and cost of telemedicine services for injured employees in Texas.
Published: October 2021 by the Workers' Compensation Research & Evaluation Group.





For more information, contact: WCResearch@tdi.texas.gov